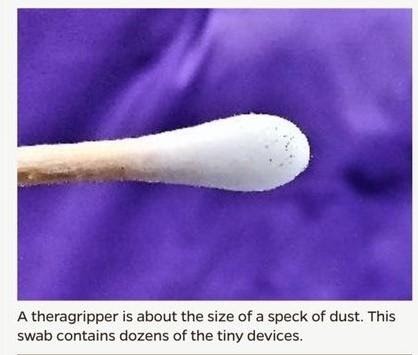
Super Immunity: What Are the Most Effective Natural Antibiotics?
November 22, 2023Nature has provided thousands of natural medicines and natural antibiotics over millennia. Most people are unaware, but many pharmaceutical medications are derived from.
- 0
- 1,088 views